Florida OIR Wants More Data, Warns Insurers about Concurrent Causation Denials
Insurance Journal
FEBRUARY 23, 2025
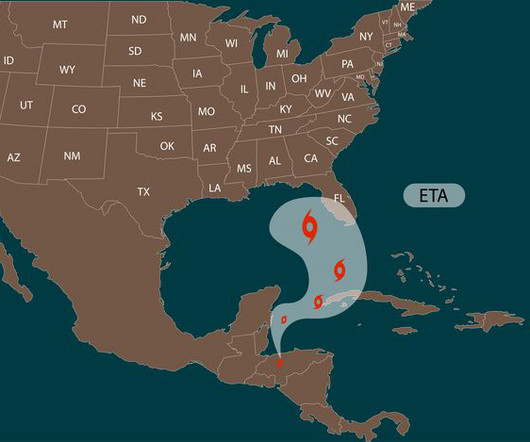
As consumer complaints have apparently mounted over unpaid hurricane losses, Florida’s top insurance regulator and some lawmakers are signaling new scrutiny on insurance carriers’ claims-handling and other practices.












































Let's personalize your content